What is Diabetes Mellitus
Diabetes mellitus is a syndrome of chronic high blood glucose levels (hyperglycemia). Although patients can live a healthy lifestyle, its complications can result in reduced life expectancy. It also causes an increase in health costs. So, it is always better to prevent or control it before the severe results. This article will help you to identify the early signs of diabetes, treatments and the method used to diagnose diabetes mellitus.
Signs of Diabetes Mellitus
Symptoms of diabetes mellitus may present as asymptomatically. So, anyone above 40 years old need to do a regular blood sugar check to detect diabetes mellitus. (Even they haven’t any of the below symptoms)
- Following symptoms are the most common among the patient
- Sudden thirst
- Weight loss
- Increased urine frequency
- Lack of energy
- Visual blurring (due to glucose-induced change in the eye lens refraction) pruritus valve or balanitis.
- Heart attack
- Erectile dysfunction
- Tingling and numbness in the feet
Early detection of diabetes signs is the best way to take action to prevent diabetes.
Complications of Diabetes Mellitus
The complications of diabetes mellitus can be divided into two main sections as Macro-vascular disease and Micro-vascular disease.
- Macro-vascular disease
- e.g.- Coronary artery disease (Heart attack)
- e.g.- Peripheral vascular disease
- e.g.- Stroke
- Micro-vascular disease
- e.g.- Diabetic retinopathy (Eye vision reduce and blindness)
- e.g.- Diabetic nephropathy (End-stage kidney disease)
- e.g.- Diabetic neuropathy (Nerves conduction reduce. So, numbness in limbs)
In a healthy person, the blood glucose level is regulated around 63-144 mg/dl (3.5-8 mmol/l) despite the varying demands of foods, fasting, and exercise.
In Diabetic Mellitus, body insulin hormone level decreases or unable to uptake by body tissue. Insulin regulates blood glucose levels. In fasting, insulin regulates glucose by releasing it from the liver. After taking a meal, the blood sugar level increases due to the digestion of the meal. So, after the meal, insulin promotes glucose uptake by fat tissue and keeps blood glucose at a constant level.
- Poor control of blood glucose level leading to diabetes mellitus causing,
- Heart attack (Cardiovascular disease)
- Kidney failure (Renal failure)
- Infections
- Strokes
- Amputation of feet due to non-healing wounds
- Blindness due to cataract neuron function and structure disrupt can occur.
Also, when a pregnant mother has poorly controlled blood sugar, the baby (fetus) becomes larger. Fetus hypoglycemia (reduced blood sugar) occurs, which leads to maldeveloped organs of the fetus. So, in diabetes mellitus, patients should take care of their complications and always try to prevent harmful consequences.
How to prevent Diabetes Mellitus
By daily inspecting, the patient should take care of their feet to prevent non-healing wounds, which can lead to amputation. Moisturizing dry skin, Check shoes inside and out for sharp bodies lead to occur non-healing ulcers, and keep feet away from sources of heat can help to prevent causing wounds.
- Also, people in risk of Diabetes Mellitus should modify their diet as,
- Low in sugar diet
- High starchy carbohydrate diet
- High fiber diet
- Low-fat diet
High starchy carbohydrate diet digests slowly. So, it does not add a large amount of glucose to blood at once.
Also, exercising regularly and keeping the body weight in the normal range is the best practice. Smokers with diabetes have higher risks for kidney and heart disease. Therefore, it’s mandatory to stop smoking to prevent the harmful effects of diabetes
By doing those things can prevent and delay the onset of diabetes mellitus. But unfortunately, it can’t cure. But fortunately, it can prevent.
How to Diagnose Diabetes
To diagnose diabetes, we can use physical examination and laboratory tests. Being positive in a single laboratory test or favorable only in clinical symptoms don’t count as diabetes mellitus. Diabetes is diagnosed as a combination of clinical signs, laboratory tests, and physical examinations are simultaneously used.
By Physical examing the patient
Patients will have symptoms of weight loss and dehydration. Older patients with diabetes will present symptoms, such as poor vision and acanthosis nigricans. The blackish color of the skin in the back of the neck and armpit is called acanthosis nigricans. It occurs due to the severe resistance by cells to insulin.
By Laboratory Diagnosis
- There are four laboratory tests use in diabetes mellitus detection. They are,
- Fasting plasma glucose > 7 mmol/l (126 mg/dl)
- Random plasma glucose > 11.1 mmol/l (200 mg/dl)
- HbA1c > 6.5 (48 mmol/mol)
- Postprandial blood glucose
- In the fasting plasma glucose test, an overnight fasting blood sample is used for the testing. If the test results indicate more than 126 mg/dl of blood glucose, it considers as positive for diabetes.
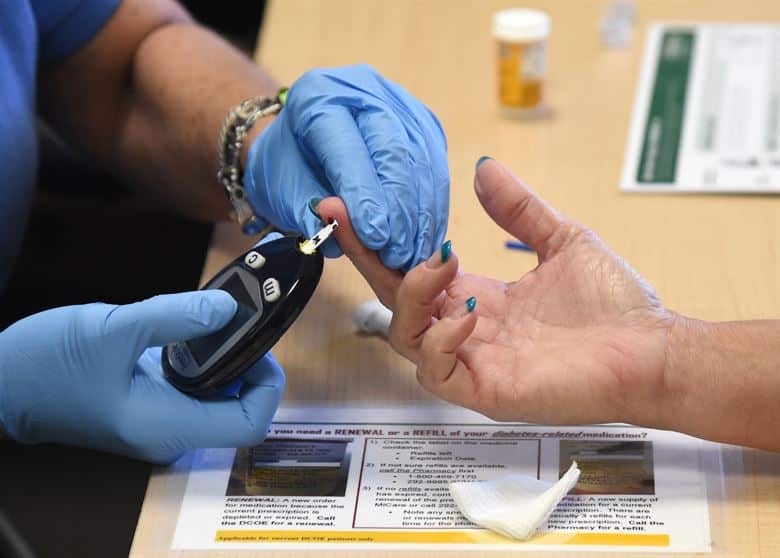
- In the random plasma blood glucose test, a blood sample is taken at a random time. It is done by pricking the finger to draw a small amount of blood. There is no need for fasting to this test. If this test result indicates the glucose level higher than 200mg/dl, it is considered positive for diabetes.
- HbA1c is a form of hemoglobin that attaches to sugar. It is used to measure a three-month average blood sugar level because red blood cells contained hemoglobin, and their life span is three months. After three months, red blood cells degrade. So this test uses not only to diagnose diabetes but also asses glycemic control in diabetes patients. If the test result is more than 6.5 is considered positive for diabetes.
- Postprandial blood glucose is a blood test that measures blood sugar levels after 2 hours of food consumption. It is considered normal if the result is less than 140 mg/dl. If the result is more than 200mg/dl, it is deemed to be positive for diabetes. Between 140 to 200 known as impaired glucose tolerance stage. If a patient is in this range, they must take extra precautions to avoid diabetes because there is a risk to have diabetes mellitus in sooner or later.
Clinical Symptoms
- A patient is considered as Diabetes mellitus positive if they present the following clinical symptoms
- Excessive urination
- Excessive thirst
- Weight loss
- Erectile dysfunction
- Infections
Even though a patient positive for one of the above tests, they are not diagnosed as diabetics.
- For the diagnosing purpose, the following criteria are used
- The presence of one of the above laboratory tests positive with the above clinical symptoms OR
- Two laboratory tests positive without clinical presentations
HbA1c is more diagnostic than other laboratory tests. For example, many people detect as healthy for glucose tolerance testing. But they are accurately identified as diabetic positive using the HbA1c test.
Treatments for diabetes mellitus
- There are three types of treatment. They are,
- Diet and lifestyle modification
- Tablet treatments
- Insulin treatment
The type of treatment depends on the diabetes type. There are many types of diabetes. But the most common types are,
- Type 1 diabetes
- Type 2 diabetes
In type 1, body insulin production failed due to the destruction of the pancreas beta cells. So in type one diabetes, insulin hormones need to give from the exterior to the body.
In type 2, there is insulin in the body. But insulin unable to enter the cells of the tissues due there to insulin resistance. So, in type 2, diabetes treatment is focused on reducing insulin resistance. But in the later stage of type 2 diabetes, most of the insulin secretion cells will be destroyed. In that stage, tablet treatments became no longer valid. So, insulin treatment will be the last option.
Tablet treatment for type 2 diabetes
The first treatment of diabetes is diet and lifestyle modification. It is hard to archive success by only taking tablets without modifying diet and lifestyle. So, while receiving tablet treatment, the patient needs to change diet and lifestyles. There are seven types of tablets. They are,
- Biguanide
- e.g., Metformin
- Sulfonylureas
- e.g., Tolbutamide
- Glibenclamide
- Glipizide and Glimepiride
- Gliclazide
- Chlorpropamide
- Meglitinides
- Thiazolidinediones
- Dipeptidyl peptidase (DPP4) inhibitors
- Acarbose
- Orlistat
Metformin
It is the best and primary treatment for diabetes. It reduces the release of glucose to the blood, which is stored in the liver.
Additional to the glucose controlling effect of Metformin, it reduces microvascular risk and beneficial in reducing heart attack (cardiovascular risk)
Sulfonylureas
Insulin produced by β cells of the pancreas. Sulfonylureas act on β cells and promote the increase of insulin secretion.
Meglitinides
Meglitinides also work on β cells of the pancreas. They are responsible for insulin secretion and improve insulin secretion in response to meals.
Thiazolidinediones
It reduces insulin resistance and enhances glucose uptake by tissues. But this drug has serious side effects like liver function failure and increase cardiovascular risk (Heart disease)
Dipeptidyl Peptidase – 4 inhibitors
- e.g., Linagliptin
- Saxagliptin
- Sitagliptin
- Vildagliptin
Dipeptidyl Peptidase – 4 inhibitors enhance the incretin effect. Incretin is a hormone, which is responsible for the secretion of insulin from the pancreas. This incretin secretion occurs as a response to the food. But the incretin effect decrease in type 2 diabetes. So this drug is most effective in the early stage of type 2 diabetes. Because insulin secretion is relatively preserved at the initial stage.
Acarbose
It reduces the absorption of dietary carbohydrates. So, blood glucose from the digesting carbohydrate will reduce.
Orlistat
It reduces the absorption of fat from the diet. So, it causes weight loss, which indirectly helps to control diabetes.
What you should know about insulin treatment
- There are three types of insulin. They are,
- Short-acting insulin
- Long-acting insulin
- Intermediate-acting insulin
The effect of short-acting insulin lasts for a small period. But it can drastically reduce the blood glucose level. Accordingly, intermediate-acting and long-acting insulin affect the blood glucose level.
Syringes are used to inject insulin into the body. Insulin syringes marked in units as 100U = 1 ml. The needles used to inject insulin should be very fine and sharp, and it should insert to its full length.
The needle is administered to fat tissue. It is located below the skin and above the muscles. Common areas of administration are the abdomen(belly), thighs, and upper arm. Insulin absorption is more rapid in the abdomen(belly) and slowest in the thigh.
When administering insulin, the body site should change regularly. Otherwise, fatty lumps in that area will develop.
Complications of insulin therapy
- At the injected site
- Painful
- Reddened lesions
- Scaring
- Abscesses occur (very rare)
- Local allergic response (resolve spontaneously)
- Fatty lumps develop due to overuse of a single injection site

Very good article.simple language is understandable
MedFog helped me in understanding my grandmother’s diabetes issues, Thank you. Hope you heal quickly! Kiss you all!
Medfog It help me to improve my knowledge about diabetes and precautions should take to prevent it. Thank you medfog
Pingback: COVID - 19 | All you need to know about Noval Coronavirus
Pingback: What is Appendicitis - How to Diagnosis of appendicitis - MedFog
Pingback: Hemosiderin staining - Skin Condition - Causes, Symptoms, and Treatment
Pingback: Ulcers - Identification and Treatment of Different Types of Ulcers
Pingback: Ceylon Cinnamon - True Cinnamon - Ceylon Extract
Pingback: Ceylon Black Pepper - Piper nigrum - Ceylon Extract
Pingback: Ceylon Cinnamon Health Benefits and Uses - Ceylon Extract